Radiology:锰与钆的对决--谁才是MR对比剂王座的主人?
2017-12-30 shaosai MedSci原创
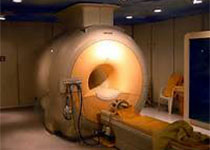
本研究旨在比较锰磁共振(MR)对比剂Mn-PyC3A与钆MR对比剂Gd-DTPA的血管内强化效果,评价Mn-PyC3A的排泄、药物动力学参数和代谢,并将结果发表在Radiology上。
本网站所有内容来源注明为“williamhill asia 医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于williamhill asia 医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“williamhill asia 医学”。其它来源的文章系转载文章,或“williamhill asia 号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与williamhill asia 联系,williamhill asia 将立即进行删除处理。
在此留言









学习谢谢分享!
79
不错的.临床在用吗?
84
学习了.谢谢分享
79
学习了感谢分享
77
henhao
89
谢谢分享.学习了
47
学习谢谢分享
42
学习了.涨知识
41
希望更少的副作用
34
学习了新知识
30