三阴性乳腺癌只能化疗?这些治疗手段指日可待
2018-08-17 光亚 医学界肿瘤频道
三阴性乳腺癌(TNBC),医生听闻这个诊断,几乎都会皱眉,相比其他亚型,它的治疗手段较少,化疗是唯一有效的治疗方式。这种特殊亚型,因雌激素受体(ER)、孕激素受体(PR)和人类表皮生长因子受体(HER2)这三个靶点均为阴性表达,让医生无从下手。雪上加霜的是,三阴性乳腺癌占所有乳腺癌的10%-16%,发病年龄较非TNBC小,局部复发和远处转移快,死亡率高,目前无针对TNBC的系统的治疗威廉亚洲博彩公司 ,没
本网站所有内容来源注明为“williamhill asia 医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于williamhill asia 医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“williamhill asia 医学”。其它来源的文章系转载文章,或“williamhill asia 号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与williamhill asia 联系,williamhill asia 将立即进行删除处理。
在此留言




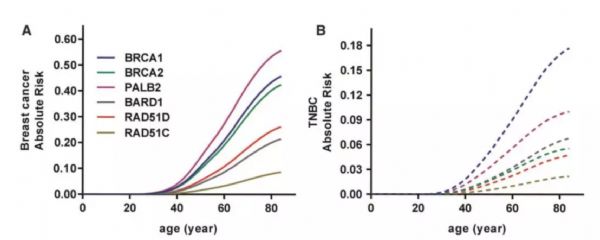






#阴性乳腺癌#
58
学习了~?
107
乳腺癌的治疗。
1
#三阴性#
46
谢谢分享学习
93
希望能有更大突破
86
学习了谢谢
108